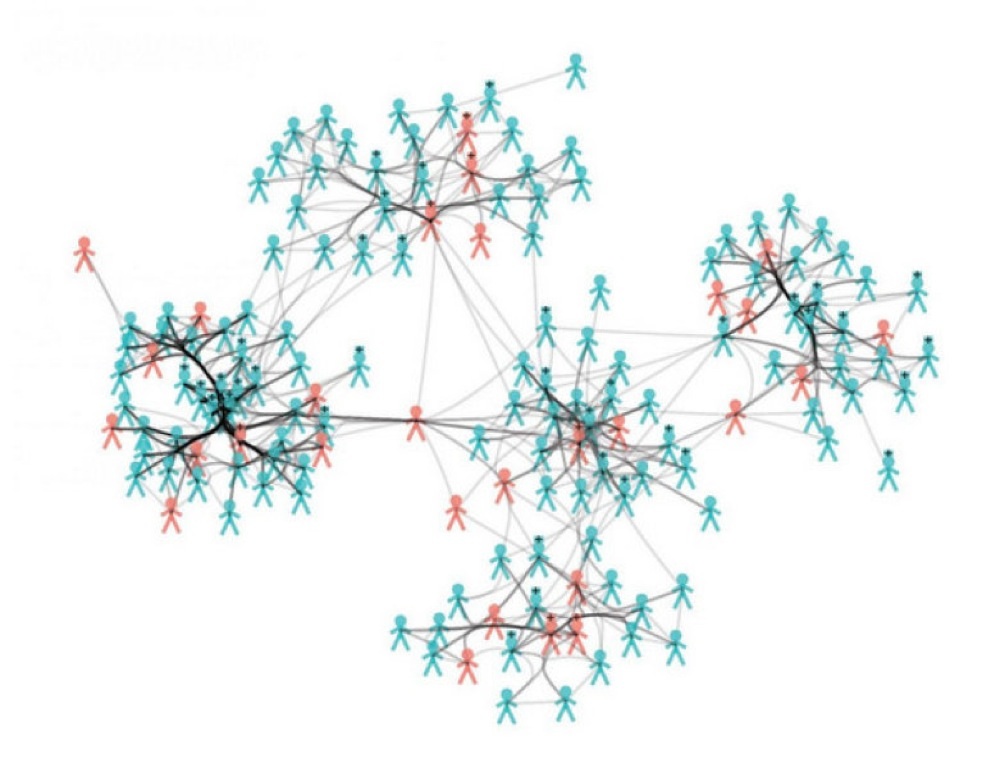
Hospital germs endanger patients. To understand their distribution and prevent a spreading in the future, French researchers have traced the ways of MRSA-germs in real time. With wireless sensors they recorded all personal contacts. Conclusion of the recently published study (Plos Computational Biology): Contact networks inform on the risk of transmission and thus warrant a more systematic study of in-hospital contact patterns. Contacts with medical staff are more „at risk“ than with other patients. With Thomas Obadia from the Université Pierre & Marie Curie spoke Carola Timmel.
Mr. Obadia, you were monitoring the interactions of MRSA-germs by wireless sensors applicated on the healthcare workers (HCWs). The analyses showed that the contact between staff and patients was riskier than the contact among one another. Why did you examine MRSA (methicillin-resistant staphylococcus aureus) and not for example Clostridium difficile?
We examined MRSA as it is commonly found in healthcare facilities and responsible for many nosocomial infections. Furthermore, it is easily transmitted during close-proximity interactions (involving physical contacts, most likely). In comparison, Clostridium difficile is transmitted by fecal-oral route and can colonize the inanimate environment for extended periods of time: transmission routes are harder to determine and may not relate to interindividual contacts as much as in the case of MRSA.
The fact, that the contact to hospital staff is more dangerous than the contact to other patients is amazing. What consequences has this knowledge regarding the change of behaviour of the hospital staff? And how can the electronic sensors help to identify the so called “superspreaders”?
We actually confirm with our data what has been extensively discussed in prior theoretical studies (namely, the role played by HCWs in shaping transmission routes), since we do have carriage data available. Regarding the change in behaviour of hospital staff, we are currently working on it. We’re trying to use these data to test prevention measures or identify individual at increased risk of spreading MRSA. While it’s still work in progress, the idea is that these kinds of networks can help identify nodes (individuals) whose behaviour affects transmissibility more than other persons: prevention measures targeting these individuals could help contain outbreaks, for example. But again, it’s still a work in progress.
What are the next steps? Are you planning some further examinations, based on the required results?
We’ve also published a second paper in Infection Control & Hospital Epidemiology a couple days ago, using the same data. In this paper, we quantify how some contact patterns can affect the risk of transmission (duration of contact, status of the individual contacted…). It’s not yet a “prevention measures” paper, but we’re still working on that.